Prompt Emergency Dentistry in Pasco, WA
Dental emergencies are quite frightening and often painful. Prompt treatment is almost always required to alleviate pain and to ensure the teeth have the best possible chance of survival.
Sometimes teeth become fractured by trauma, grinding or biting on hard objects. In other cases, fillings, crowns and other restorative devices can be damaged or fall out of the mouth completely. If there is severe pain, it is essential to make an appointment with the dentist as quickly as possible. The pain caused by dental emergencies almost always gets worse without treatment, and dental issues can seriously jeopardize physical health.
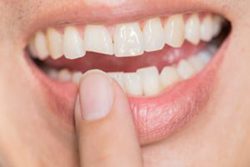
Cracked and fractured teeth are common dental problems. As people retain their natural teeth longer (due to advances in dental technology), the likelihood of cracked teeth increases. There are many reasons why teeth may crack, for example, biting on hard objects, trauma, grinding and clenching of teeth. All of these behaviors place the teeth under extra strain and render them more susceptible to cracking.
When tooth enamel is cracked, pain can become momentarily debilitating. When no pressure is exerted on the crack there may be no discomfort. However, as the cracked tooth performs a biting action, the crack widens. The pulp and inner workings of the tooth then become exposed, and painful irritation occurs. As pressure is released again, the two parts of the crack fuse back together, and pain subsides. If left untreated, the pulp becomes irreversibly damaged and constantly painful. The resulting pulp infection can affect the bone and soft tissue surrounding the tooth.
Symptoms of a cracked tooth may include:
- Unexplained pain when eating.
- Sensitivity to warm and cold foods.
- Pain with no obvious cause.
- Difficulty pinpointing the location of the pain.
What kind of cracks can affect the teeth?
There are many ways in which a tooth can be cracked. The specific type of crack will determine what type of treatment is viable. In many cases, if the crack is not too deep, root canal therapy can be performed and the natural tooth can remain in the mouth. In other situations, the tooth is too badly damaged and requires extraction.
Here is a brief overview of some of the most common types of cracks:
Crazes – These are generally tiny vertical cracks that do not place the teeth in danger. These scratches on the surface of the teeth are considered by most dentists to be a normal part of the tooth anatomy. A craze rarely requires treatment for health reasons, but a wide variety of cosmetic treatments can be performed to reduce the negative aesthetic impact.
Oblique supragingival cracks – These cracks only affect the crown of the tooth and do not extend below the gum line. Usually, the affected part of the tooth will eventually break off. Little pain will result, because the tooth pulp (that contains the nerves and vessels) will remain unaffected.
Oblique subgingival cracks – These cracks extend beyond the gum line, and often beyond where the jawbone begins. When a piece breaks off, it will usually remain attached until the dentist removes it. Oblique subgingival cracks are painful and may require a combination of periodontal surgery (to expose the crown), and endodontic treatment to place a crown or other restorative device.
Vertical furcation cracks – These cracks occur when the roots of the tooth separate. This type of crack almost always affects the nerve of the tooth. Because the tooth will not generally separate completely, root canal therapy and a crown can usually save the tooth.
Oblique root cracks – These cracks tend not to affect the surface of the tooth at all. In fact, the damage is only apparent below the gum line and usually below the jawbone. Root canal therapy may be possible; depending on how close the fracture is to the tooth surface. However, extraction is almost always the only option after sustaining this classification of fracture.
Vertical apical root cracks – These cracks occur at the apex (tip of the root). Though the tooth does not require extraction from a dental perspective, many patients request an extraction because of the high degree of pain. Root canal therapy alleviates the discomfort for a while, but most often, teeth affected by such cracks are eventually extracted.
How are cracks in the teeth treated?
There are many different types of cracked teeth. Some can only be exposed using X-ray machines, while others are clearly visible to the naked eye. In cases where the tooth root is affected, root canal therapy is the most viable treatment option. The pulp, nerves and vessels of the tooth will be removed, and the resulting space will be filled with gutta-percha. A crown or filling will be added to stabilize the tooth and it will continue to function as normal.
When the crack is too severe for the tooth to be saved, the dentist will perform an extraction. There are a number of restorative options in this case, such as bridges, dental implants and partial dentures. All of these structures can restore biting, chewing and speaking functions.

Dental emergencies are quite frightening and often painful. Prompt treatment is almost always required to alleviate pain and to ensure the teeth have the best possible chance of survival.
Sometimes teeth become fractured by trauma, grinding or biting on hard objects. In other cases, fillings, crowns and other restorative devices can be damaged or fall out of the mouth completely. If there is severe pain, it is essential to make an appointment with the dentist as quickly as possible. The pain caused by dental emergencies almost always gets worse without treatment, and dental issues can seriously jeopardize physical health.
Types of dental emergency and how to deal with them
Avulsed tooth (tooth knocked out)
If a tooth has been knocked clean out of the mouth, it is essential to see a dentist immediately. When a tooth exits the mouth, tissues, nerves and blood vessels become damaged. If the tooth can be placed back into its socket within an hour, there is a chance the tissues will grow to support the tooth once again.
Here are some steps to take:
- Call the dentist.
- Pick up the tooth by the crown and rinse it under warm water. DO NOT touch the root.
- If possible, place it back into its socket – if not tuck it into the cheek pouch.
- If the tooth cannot be placed in the mouth, put the tooth into a cup of milk, saliva, or water as a last resort. It is important to keep the tooth from drying out.
- Get to the dentist, quickly and safely.
The dentist will try to replace the tooth in its natural socket. In some cases, the tooth will reattach, but if the inner mechanisms of the teeth are seriously damaged, root canal therapy may be necessary.
Lost filling or crown
Usually, a crown or filling comes loose while eating. Once it is out of the mouth, the affected tooth may be incredibly sensitive to temperature changes and pressure. Crowns generally become loose because the tooth beneath is decaying. The decay causes shape changes in the teeth – meaning that the crown no longer fits.
If a crown has dropped out of the mouth, make a dental appointment as soon as possible. Keep the crown in a cool, safe place because there is a possibility that the dentist can reinsert it. If the crown is out of the mouth for a long period of time, the teeth may shift or sustain further damage.
When the dentist is not immediately accessible, here are the steps to take:
- Apply clove oil to the tooth to alleviate pain.
- Clean the crown and affix it onto the tooth with dental cement. This can be purchased at the local pharmacy.
- If the crown is lost, smear the top of the tooth with dental cement to alleviate discomfort.
- DO NOT use any kind of glue to affix the crown.
The dentist will check the crown to see if it still fits. If it does, it will be reattached to the tooth. Where decay is noted, this will be treated and a new crown will be made.
Cracked or broken teeth
The teeth are strong, but they are still prone to fractures, cracks and breaks. Sometimes fractures are fairly painless, but if the crack extends down into the root, it is likely that the pain will be extreme. Fractures, cracks and breaks can take several different forms, but are generally caused by trauma, grinding and biting. If a tooth has been fractured or cracked, there is no alternative but to see the dentist as quickly as possible.
Where a segment of tooth has been broken off, here are some steps that can be taken at home:
- Call the dentist.
- Rinse the tooth fragment and the mouth with lukewarm water.
- Apply gauze to the area for ten minutes if there is bleeding.
- Place a cold, damp dishtowel on the cheek to minimize swelling and pain.
- Cover the affected area with over-the-counter dental cement if there is no way to see the dentist immediately.
- Take a topical pain reliever.
The nature of the break or fracture will limit what the dentist is able to do. If a fracture or crack extends into the root, root canal therapy may be the only effective way to retain the tooth. In the case of a complete break, the dentist will usually affix the fragment back onto the tooth as a temporary measure.
Dislodged/loose teeth
When a tooth has been dislodged or loosened from its socket by trauma or decay, it might be possible to save it. If the tooth remains in the mouth and attached to the blood vessels and nerves, there is a good chance root canal therapy will not be necessary.
It is important to call the dentist immediately to make an appointment. In the meantime, use a cold compress and over-the-counter medications to relieve pain. The dentist will reposition the tooth and add splints to stabilize it. If the tooth fails to heal, root canal therapy may be required.
In the past, if you had a tooth with a diseased nerve, you’d probably lose that tooth. Now, with “root canal therapy,” your tooth can be saved. When a tooth is cracked or has a deep cavity, bacteria can enter the pulp tissue and germs can cause an infection inside the tooth. If left untreated, an abscess may form. If the infected tissue is not removed, pain and swelling can result. This can injure your jawbones and be harmful to your overall health.
Root canal therapy involves one to three visits. During treatment, your general dentist or endodontist removes the affected tissue. Next, the interior of the tooth will be cleaned and sealed. Finally, the tooth is filled with a dental composite. If your tooth has extensive decay, your dentist may suggest placing a crown to strengthen and protect the tooth from breaking. As long as you continue to care for your teeth and gums with regular brushing, flossing, and checkups, your restored tooth can last a lifetime.
What is a root canal procedure?
Tooth decay can progress down into the pulp. When this happens, the pulp can become infected. Infection of the pulp can be very painful and can also deteriorate into an abscessed tooth when infection and swelling develops in the tissues around or beneath the tooth. When the pulp becomes infected or the tooth becomes abscessed, it is necessary to perform a root canal.
Why do I feel pain?
When the pulp becomes infected due to a deep cavity or fracture, bacteria can seep in. When there has been an injury due to trauma, the pulp can die. Damaged or dead pulp causes increased blood flow, pressure, and cellular activity. Pain in the tooth is commonly felt when biting down or chewing, and eating or drinking hot and/or cold foods and beverages.
Why do I need root canal therapy?
The tooth will not heal by itself. Without treatment, the infection will spread. The bone around the tooth will begin to degenerate, and the tooth may fall out. Pain usually worsens until one is forced to seek emergency dental attention. The only alternative is extraction of the tooth, which can cause the surrounding teeth to shift, resulting in a bad bite. Though an extraction is cheaper, the space left behind will require an implant or a bridge, which can be more expensive than root canal therapy. If you have the choice, it’s always best to keep your original teeth.
What are the risks and complications with root canal therapy?
More than 95 percent of root canal therapies are successful. However, sometimes a case needs to be redone due to diseased canal offshoots that went undetected, or the fracturing of the canal filling. More commonly, a root canal therapy will fail altogether, marked by the return of pain.
What happens after root canal therapy?
Once root canal therapy is completed, the endodontist will refer the patient back to our office for the permanent restoration on the tooth. A temporary filling was placed immediately following the root canal therapy and will need to be replaced with a permanent filling or crown and build up. A crown will be necessary on all posterior teeth to properly protect the root canal- treated tooth from fracturing. Front teeth can typically be restored with a filling, however a crown may be necessary in some cases. Your dentist will determine the best choice for your individual needs.
How long will the restored tooth last?
Your restored tooth could last a lifetime, if you continue to care for your teeth and gums. However, regular checkups are necessary. As long as the root(s) of a treated tooth are nourished by the tissues around it, your tooth will remain healthy.
How does root canal therapy save my tooth?
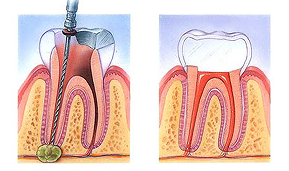
- An opening is made through the crown of the tooth into the pulp chamber.
- The pulp is removed, and the root canals are cleaned, enlarged and shaped.
- Medications may be put in the pulp chamber and root canal(s) to help get rid of germs and prevent infection.
- A temporary filling will be placed in the crown opening to protect the tooth between dental visits. Your dentist may leave the tooth open for a few days to drain. You might also be given medicine to help control infection that may have spread beyond the tooth.
- The temporary filling is removed and the pulp chamber and root canal(s) are cleaned and filled.
- In the final step, a gold or porcelain crown is usually placed over the tooth.

Third molars, commonly referred to as wisdom teeth, are usually the last four of 32 teeth to erupt (surface) in the mouth, generally making their appearance between the ages of 17 to 25. They are located at the back of the mouth (top and bottom), near the entrance to the throat. The term “wisdom” stems from the idea that the molars surface at a time typically associated with increased maturity or “wisdom”.
In most cases, inadequate space in the mouth does not allow the wisdom teeth to erupt properly and become fully functional. When this happens, the tooth can become impacted (stuck) in an undesirable or potentially harmful position. If left untreated, impacted wisdom teeth can contribute to infection, damage to other teeth, and possibly cysts or tumors.
There are several types, or degrees, of impaction based on the actual depth of the teeth within the jaw:
Soft Tissue Impaction: The upper portion of the tooth (the crown) has penetrated through the bone, but the gingiva (gum) is covering part or all of the tooth’s crown and has not positioned properly around the tooth. Because it is difficult to keep the area clean, food can become trapped below the gum and cause an infection and/or tooth decay, resulting in pain and swelling.
Partial Bony Impaction: The tooth has partially erupted, but a portion of the crown remains submerged below the gum and surrounding jawbone. Again, because it is difficult to keep the area clean, infection will commonly occur.
Complete Bony Impaction: The tooth is completely encased by jawbone. This will require more complex removal techniques.
Reasons to remove wisdom teeth
While not all wisdom teeth require removal, wisdom teeth extractions are most often performed because of an active problem such as pain, swelling, decay or infection, or as a preventative measure to avoid serious problems in the future. If impaction of one or more wisdom teeth is present, and left untreated, a number of potentially harmful outcomes can occur, including:
- Damage to nearby teeth: Second molars (the teeth directly in front of the wisdom teeth) can be adversely affected by impacted wisdom teeth, resulting in tooth decay (cavities), periodontal disease (gum disease) and possible bone loss.
- Disease: Although uncommon, cysts and tumors can occur in the areas surrounding impacted wisdom teeth.
- Infection: Bacteria and food can become trapped under the gum tissue, resulting in an infection. The infection can cause considerable pain and danger.
- Tooth Crowding: It has been theorized that impacted wisdom teeth can put pressure on other teeth and cause them to become misaligned (crowded or twisted). This theory isn’t universally accepted by all dental professionals, and it has never been validated by any scientific studies.
Wisdom teeth examination
As with any dental procedure, your dentist will want to initially conduct a thorough examination of the wisdom and surrounding teeth. Panoramic or digital X-rays will be taken in order for your dentist to evaluate the position of the wisdom teeth and determine if a current problem exists, or the likelihood of any potential future problems. The X-rays can also expose additional risk factors, such as deterioration or decay of nearby teeth. Early evaluation and treatment (typically in the mid-teen years) is recommended in order to identify potential problems and to improve the results for patients requiring wisdom teeth extractions. Only after a thorough examination can your dentist provide you with the best options for your particular case.
What does the removal of wisdom teeth involve?
Wisdom teeth removal is a common procedure, generally performed under local anesthesia, intravenous (IV) sedation, or general anesthesia by a specially trained dentist in an office surgery suite. The surgery does not require an overnight stay, and you will be released with post-operative instructions and medication (if necessary), to help manage any swelling or discomfort.
